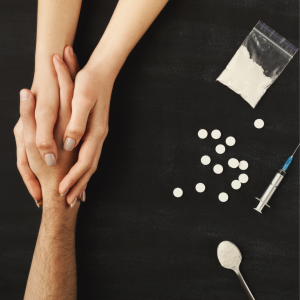
David is living with hepatitis B, and he spoke about empathy and mental health as a panelist at the World Hepatitis Summit (WHS) 2024
Another World Hepatitis Summit (WHS) has come and gone, this time in Lisbon, Portugal. I previously attended the 2022 summit in Geneva and spoke during the Youth Can’t-Wait and Closing Sessions. I would like to give my thanks to the wonderful people at the World Hepatitis Alliance, for allowing me to travel and speak at this year’s summit as well.
I spoke during a newly created session called Hepatitis and Mental Health. During this session, a video I made in collaboration with the WHA last year, was played before I spoke. It is part of the WHA “I can’t wait” series of videos, which showcase patient advocates and their journeys with patient advocacy and why they can’t wait for a world without hepatitis. I, the dedicated and powerful Shabana Begum of the UK, and the courageous and vocal Shaibu Issa of Tanzania are the first to be featured in these videos.
I can’t wait… these words evoke dire urgency. During this summit, I felt and heard the urgency from many of the speakers, advocates, and attendees. From the opening session, it was emphasized that the world DOES have the tools and resources but DOES NOT have the required amount of political and social will to eliminate viral hepatitis by 2030. The need for person-centered and culturally appropriate approaches as being critically important was also highlighted.
These declarations capture the moment the viral hepatitis community is currently in. Time is slipping away by the day and the people who suffer from viral hepatitis, hepatitis B and D included, cannot continue to wait in silence as they have been. Deaths from hepatitis B are still alarmingly high each year. These statistics highlight a problem of stigma and discrimination that presents differently depending on where you are located or who you are talking to. Stigma and discrimination can cause mental health problems and prevent millions of people living with hepatitis from finding their voice, feeling comfortable sharing their story, and being diagnosed. Without solving this multi-faceted problem, the goal of eliminating viral hepatitis by 2030 is just an empty platitude.
Having the privilege and platform to speak about hepatitis and mental health during this summit was very important to me. My struggles with hepatitis B and my mental health struggles are interconnected in so many ways. That is also true for so many other patients who have struggled with poor mental health. Long before I started my patient advocacy journey, I felt voiceless. Long before I ever talked publicly about my mental health struggles, I felt voiceless.
Empathy is a crucial piece of the puzzle for how we give those who feel voiceless the greatest opportunity to find their voice, regardless of where they are from or the stigmas that surround them. We must be empathetic when creating policies, action plans, and declarations. So many millions of people are left undiagnosed, untreated, and voiceless because of fear of the societal, associative, and personal stigma that they will go through if they seek out a diagnosis or talk about their status openly. There is still so much misinformation surrounding hepatitis and the only feasible way to fight this is by amplifying the voices of those who speak the truth about hepatitis with empathy, cultural sensitivity and appropriate.
The symptoms of poor mental health exacerbate this feeling of voicelessness. After five years of advocacy, over a decade of therapy, and five years of being on a consistent treatment for my hepatitis B, I still struggle with clinical depression and anxiety. I will live every day with depression and anxiety in varying degrees for the foreseeable future. My mental health started to trend downward late last year. I had to find the strength to start an antidepressant medication and give it an honest try. I can happily say, that today and every day after will mark the longest I’ve been on an antidepressant (almost six months now), and I can report that it is helping me manage my mental health and to continue managing my hepatitis.
I say all of this to highlight the connection between times in my life where I have actively been taking steps to manage my mental health and my hepatitis B. These periods overlap with each other, and they have one important thing in common. Empathy for myself and others. This is one of the strongest coping tools I have to manage my hepatitis B and my mental health. Patient health outcomes are linked to the state of their mental health and the tools and resources they are given to help manage it.
After attending this World Hepatitis Summit, I feel a calling to act with more urgency. This isn’t an easy task. For me, it’s one of the most challenging aspects of advocacy. I have such a natural tendency to self-talk in very judgmental and negative terms. I sometimes think I’m a terrible person for not doing more and taking more time to learn how to become a more capable and productive advocate. I ask myself why I’m not having more conversations, learning about others’ perspectives, and potentially teaching someone or setting them on a path of changing their minds about hepatitis and mental health.
The desire to grow more as an advocate and connect more with others is within me, but the key to taking more action is to meet myself where I am currently and to practice self-empathy. When I speak to myself with empathy, kindness, and encouragement, I am much more likely to grow and make a positive change, even though mental health struggles.
Most people in the world can relate to or know someone who has struggled with their mental health. This commonality between people can be a powerful tool if wielded with empathy instead of fearmongering and focusing on the most rare, violent, and negative aspects of mental health struggles. These stories fill the public, media, social media, and political discourse and create more layers of stigma (public, associative, self, provider). Changing this narrative will be a monumental undertaking but to use one of my favorite quotes, “The best time to start was yesterday. The next best time is today.”
Check out David’s storytelling journey here: https://www.hepbstories.org/justb/david?rq=david