The Scenario
 Yufei Zhao is 45 years old and lives with his family in Philadelphia, Pa. Yufei discovered that he had hepatitis B when he attended a community health fair with his family. Even though he was instructed to talk about his diagnosis with a doctor and learn more about possible treatment options, Yufei decided to do nothing as he did not feel sick. While he has health insurance through his employer, he never utilizes any health care services. He often skips annual wellness visits as he says he “never gets sick.”
Yufei Zhao is 45 years old and lives with his family in Philadelphia, Pa. Yufei discovered that he had hepatitis B when he attended a community health fair with his family. Even though he was instructed to talk about his diagnosis with a doctor and learn more about possible treatment options, Yufei decided to do nothing as he did not feel sick. While he has health insurance through his employer, he never utilizes any health care services. He often skips annual wellness visits as he says he “never gets sick.”
 A few weeks ago, Yufei’s family noticed that he has been skipping meals frequently saying he’s full or not hungry. At his daughter’s urging, he decided to go for a visit. After conducting some more tests, his doctor explained that the chronic infection with the hepatitis B virus had progressed substantially, and he had developed cirrhosis. After an MRI diagnosis, it was revealed that Yufei had liver cancer.
A few weeks ago, Yufei’s family noticed that he has been skipping meals frequently saying he’s full or not hungry. At his daughter’s urging, he decided to go for a visit. After conducting some more tests, his doctor explained that the chronic infection with the hepatitis B virus had progressed substantially, and he had developed cirrhosis. After an MRI diagnosis, it was revealed that Yufei had liver cancer.
 The Hepatologist (liver doctor) explained to Yufei that the liver is an important organ and acts as a cleaning system for the body. It removes toxic waste, purifies blood, and helps to digest food properly. When the virus entered the liver, it made many copies of itself and started attacking healthy liver cells. This led to inflammation and weakened the ability of the liver to carry out its most essential tasks. Because he was never monitored for hepatitis B, the virus allowed tumors to grow in the liver which caused the cancer. When the tumors grow in size or number, it eventually spreads to other parts of the body and disrupts other vital processes as well.
The Hepatologist (liver doctor) explained to Yufei that the liver is an important organ and acts as a cleaning system for the body. It removes toxic waste, purifies blood, and helps to digest food properly. When the virus entered the liver, it made many copies of itself and started attacking healthy liver cells. This led to inflammation and weakened the ability of the liver to carry out its most essential tasks. Because he was never monitored for hepatitis B, the virus allowed tumors to grow in the liver which caused the cancer. When the tumors grow in size or number, it eventually spreads to other parts of the body and disrupts other vital processes as well.
 The doctor mentioned that liver cancer is often called the silent disease because symptoms may not always be present. Even with a hepatitis B, a person could look or feel okay but that does not mean the virus isn’t active and causing damage. When the symptoms do show up, it might be too late to prevent liver cancer. After discussing his options with the doctor, Yufei learned that the best treatment for him was to get a liver transplant.
The doctor mentioned that liver cancer is often called the silent disease because symptoms may not always be present. Even with a hepatitis B, a person could look or feel okay but that does not mean the virus isn’t active and causing damage. When the symptoms do show up, it might be too late to prevent liver cancer. After discussing his options with the doctor, Yufei learned that the best treatment for him was to get a liver transplant.
He weighed the pros and cons of getting a transplant and consulted with his family. Now, Yufei is placed on a waiting list for a liver transplant to become available. In the meantime, his doctor has suggested other methods to destroy the smaller tumors without surgery through radiation (ablation). Yufei continues to spend more time with his family as he hopes to respond well to treatment until a new or partial liver is available.
The Challenge
Cultural Perceptions on Health & Well-being
- Yufei is an older male in the household and the backbone of the family. For this reason, he considers it an obligation to prioritize his family over his personal health. It is important to understand these cultural and social beliefs prevalent in many different cultures and households.
- Family members should be advised to encourage their loved ones (especially older family members) to take charge of their health. It is important to check-in with your loved ones and assure them that sickness does not necessarily mean weakness. Taking care of one’s health can mean taking charge of one’s future.
Hep B and Liver Cancer
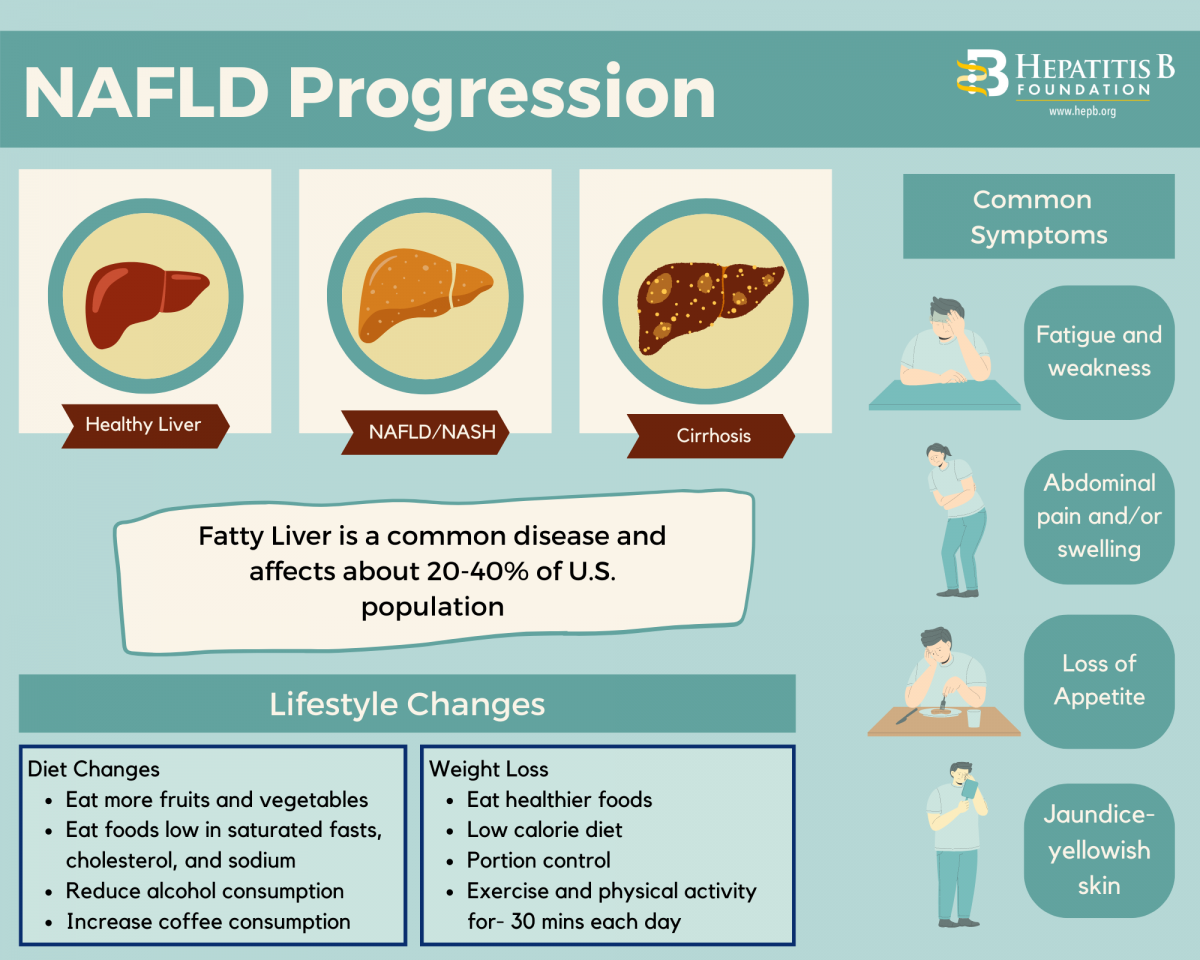
- Hepatitis B is a virus that causes inflammation of the liver. Without proper diagnosis and treatment, the virus can continue to multiply and damage healthy liver cells. This can lead to inflammation and scarring of the liver. This prevents the liver from doing its most important functions to maintain overall health which may result in the development of harmful tumors.
Liver Cancer is a Silent Disease
- Many people with hepatitis B or liver cancer do not show symptoms of sickness but that does not mean the virus isn’t present or not actively working to harm the liver. Eventually, the physical symptoms will become noticeable as the virus/cancer advances to a more dangerous stage.
What can you do?
Get tested!
- The most important thing you can do to prevent liver cancer is to get tested for hepatitis B. Most liver cancers develop from undiagnosed hepatitis B infections. There are a lot of people who have hepatitis B and do not know about it because they have never been tested. Even if you feel healthy and okay, it does not hurt to get tested!
- If you don’t have hepatitis B, the test can tell you if you are vaccinated or if you need vaccination (which can provide lifelong protection from ever getting hepatitis B and help prevent liver cancer).
Get screened!
- If you have hepatitis B, it is critical to manage the progression of the virus in your liver. For this reason, it is important to go through monitoring of your hepatitis B infection, liver health, and screen regularly for liver cancer.
- Discuss with your doctor if you are at high-risk and how often you should get screened. It is recommended to get an ultrasound every 6 months to check how the virus is impacting the liver. AFP testing may also be done with regular monitoring of the liver to check for the possibility of liver cancer.
Get educated!
- Stay up to date with the latest research and information on liver cancer! If you have hepatitis B, you should know that there is no cure for the virus but there is a lot of research that shows what you can do to ensure you live a healthy and long life.
- Take an active role in learning about the disease and how it can affect your health over time. Learn about fibrosis, cirrhosis, liver cancer staging, and available treatments for hep B infection.

References
- https://www.hepb.org/research-and-programs/liver/screening-for-liver-cancer/
- https://www.cancer.org/cancer/liver-cancer/treating/by-stage.html#:~:text=Treatment%20options%20might%20include%20ablation,%2C%20and%2For%20radiation%20therapy.
- https://www.cancer.org/cancer/liver-cancer/detection-diagnosis-staging/staging.html
- https://www.hepb.org/research-and-programs/liver/risk-factors-for-liver-cancer/